Understanding Nipah Virus Infection: A Comprehensive Guide
Stay informed about the transmission, symptoms, and prevention of the rare but severe Nipah virus.

In an increasingly interconnected world, understanding the emergence and spread of infectious diseases is more critical than ever. While global attention frequently shifts between various well-known pathogens, there are lesser-known viruses that pose significant threats due to their severity and high mortality rates. One such pathogen is the Nipah virus (NiV).
Nipah virus is a zoonotic pathogen, meaning it jumps from animals to humans, causing severe disease characterized by acute respiratory infection and fatal encephalitis. Though outbreaks have historically been localized primarily to South and Southeast Asia, the global health community closely monitors NiV because of its pandemic potential and the devastating impact it has on affected communities.
This comprehensive guide will delve deep into what the Nipah virus is, how it transmits, the clinical symptoms to watch for, current diagnostic and treatment landscapes, and the vital prevention strategies needed to protect both individuals and broader communities from this formidable biological threat.
What is the Nipah Virus (NiV)?
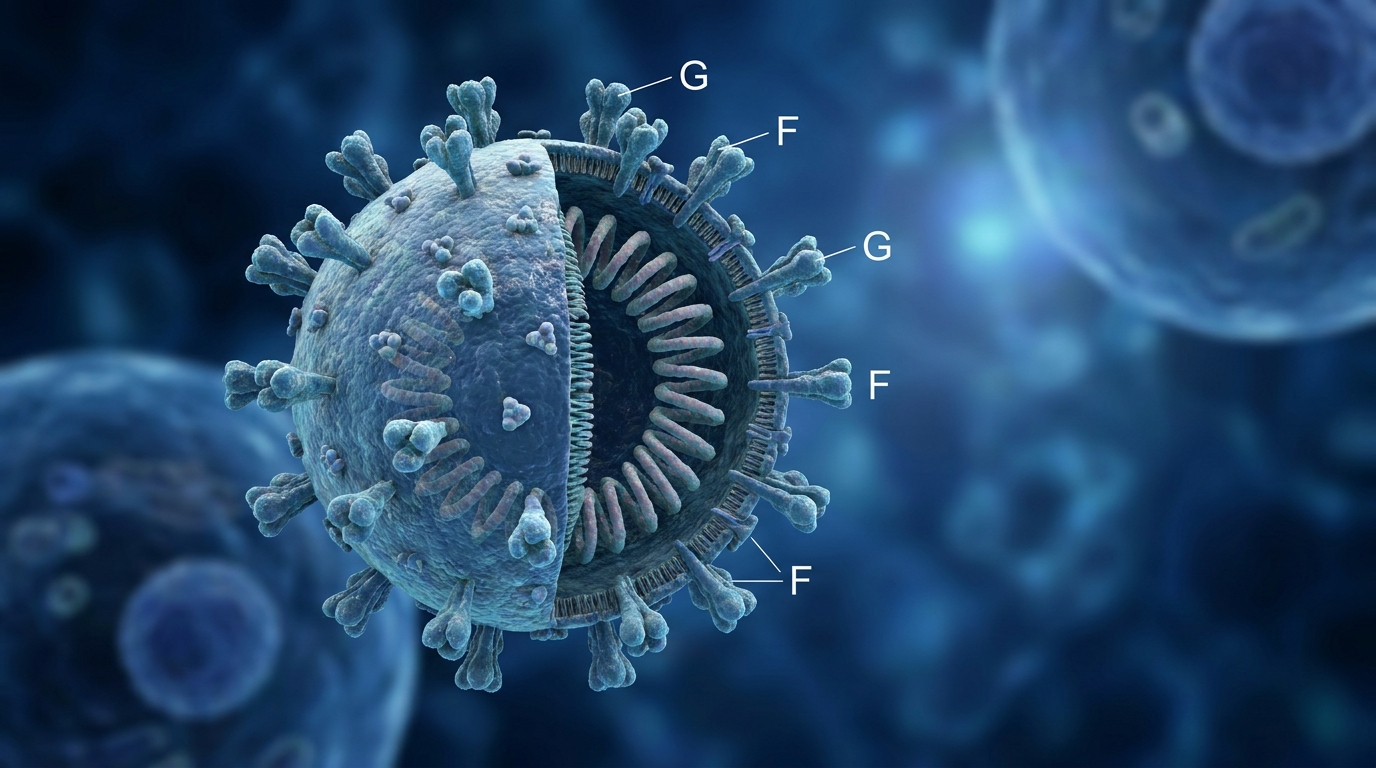
The Nipah virus (NiV) belongs to the genus Henipavirus within the family Paramyxoviridae. It is an RNA virus that is highly pathogenic to humans and certain animals. As a zoonotic virus, its lifecycle relies on animal reservoirs in the wild before an event—often driven by environmental changes or human agricultural practices—allows it to spill over into the human population.
The natural hosts of the Nipah virus are fruit bats of the Pteropodidae family, commonly known as flying foxes. These bats harbor the virus without showing clinical signs of illness, shedding the pathogen in their saliva, urine, semen, and excrement. When humans or intermediate animal hosts come into contact with these contaminated fluids, the spillover event occurs.
"Nipah virus was first identified in 1999 during an outbreak among pig farmers in Malaysia and Singapore. The virus was named after the Malaysian village, Sungai Nipah, where the first isolated strain was discovered."
During that initial 1999 outbreak, pigs served as the intermediate host. The virus spread rapidly among swine populations before infecting the farmers who handled them. This outbreak resulted in nearly 300 human cases and over 100 deaths, prompting the culling of over a million pigs to halt the spread, which caused massive economic devastation to the local agricultural sector.
Since then, outbreaks have occurred almost annually in Bangladesh and periodically in eastern India. What makes Nipah virus particularly alarming to global health organizations like the WHO is its staggering mortality rate. The fatality rate of NiV can range from 40% to 75%, depending heavily on the specific viral strain, the nature of the outbreak, and the capacity of local healthcare infrastructure to provide intensive supportive care.
Key Facts About NiV Origins:
- Zoonotic Nature: Initially transmitted from animals (bats, pigs) to humans.
- Natural Reservoir: Fruit bats (flying foxes) of the Pteropodidae family.
- First Identification: 1999, during a major outbreak among pig farmers in Malaysia and Singapore.
- High Severity: Outbreaks are relatively rare but carry a high fatality rate of up to 75%.
How Does Nipah Virus Spread?

Understanding the transmission dynamics of the Nipah virus is essential for outbreak prevention and containment. The virus has demonstrated multiple routes of transmission, making it a complex pathogen to control once it enters a human population.
The primary route of infection is direct contact with infected animals or their bodily fluids. In regions like Malaysia, this historically meant contact with infected pigs. However, in Bangladesh and India, transmission is most frequently linked directly to the natural bat reservoir. Humans can contract the virus through the consumption of food products contaminated by infected bats.
A classic and heavily documented example is the consumption of raw date palm sap. In parts of South Asia, sap is collected overnight in clay pots attached to date palm trees. Fruit bats often visit these pots to drink the sweet sap, contaminating it with their saliva or urine. When humans consume this raw sap the next morning, they ingest the live virus.
Furthermore, human-to-human transmission is a significant driver of outbreaks, particularly in healthcare settings and within families. This occurs through close physical contact with the bodily fluids, excretions, or respiratory droplets of an infected individual. Because of this, healthcare workers and family caregivers are at an exceptionally high risk of contracting the virus. Maintaining a hygienic environment is critical; while NiV is much rarer than common respiratory viruses, understanding essential cleaning tips for infection control can generally help maintain a safe environment when caring for sick individuals.
Primary Transmission Routes:
- Direct Animal Contact: Handling infected animals, such as bats or pigs, or coming into contact with their saliva, urine, or blood.
- Contaminated Food: Consuming raw date palm sap, or eating fruits that have bat bite marks or have been contaminated by bat droppings.
- Human-to-Human: Close contact with the respiratory droplets or bodily fluids of an infected person.
- Nosocomial (Hospital) Spread: Healthcare workers are at high risk if strict infection control and PPE measures are not rigorously followed.
Recognizing the Symptoms of NiV Infection
The clinical presentation of Nipah virus infection can vary widely, ranging from asymptomatic (subclinical) infection to acute respiratory distress and fatal encephalitis. The incubation period—the time from exposure to the virus to the onset of symptoms—typically ranges from 4 to 14 days, though prolonged incubation periods of up to 45 days have been reported in rare cases.
Initial symptoms are notoriously non-specific, often mimicking other common viral infections like influenza or dengue fever. Patients usually present with a sudden onset of high fever, severe headaches, muscle pain (myalgia), vomiting, and a sore throat. This non-specific early phase makes rapid clinical diagnosis incredibly challenging without a known history of exposure.
As the infection progresses, the virus aggressively attacks the respiratory and central nervous systems. Respiratory issues can escalate rapidly into atypical pneumonia and severe acute respiratory distress, leaving patients struggling to breathe. Simultaneously, the neurological impact begins to manifest. Patients may experience profound dizziness, drowsiness, and an altered state of consciousness.
In severe cases, NiV causes encephalitis—a life-threatening inflammation of the brain. This neurological decline can be incredibly rapid, progressing from mild confusion to seizures and a deep coma within 24 to 48 hours. Immediate intensive medical intervention is required to manage brain swelling and support vital functions.
Even for those who survive the acute phase of the infection, the battle is not always over. Approximately 20% of survivors are left with residual neurological consequences, such as persistent convulsions, sudden personality changes, or cognitive deficits. There are also documented cases of latent infections, where the virus reactivates months or even years later, causing delayed-onset encephalitis.
Diagnosis and Current Treatment Options

Diagnosing Nipah virus in its early stages is a significant clinical hurdle. Because the initial symptoms resemble those of many other endemic diseases in the affected regions, NiV is rarely the first suspicion unless there is an ongoing recognized outbreak. However, if clinical suspicion is raised, specific laboratory tests can confirm the presence of the virus.
During the acute and early phases of the disease, diagnosis is typically achieved using real-time polymerase chain reaction (RT-PCR) from bodily fluids such as throat and nasal swabs, cerebrospinal fluid (CSF), urine, and blood. Later in the course of the disease, or after recovery, enzyme-linked immunosorbent assay (ELISA) testing can detect specific antibodies (IgG and IgM) produced by the body's immune system in response to the virus.
When it comes to treatment, the medical community currently faces a stark reality: there are no specific antiviral drugs or vaccines approved by the FDA or WHO for the targeted treatment or prevention of Nipah virus in humans. Because of this, clinical management is entirely focused on intensive supportive care.
Supportive care involves aggressively managing symptoms as they arise. This includes administering fluids to maintain hydration, using medications to control fever and seizures, and providing mechanical ventilation for patients experiencing severe respiratory failure or deep coma. While specific treatments are lacking, maintaining a robust baseline of health is always beneficial. Discovering how to boost your immune system through diet and exercise can help ensure your body is in the best possible shape to fight off unexpected pathogens.
Additionally, prolonged hospital stays and the anxiety of outbreaks can take a massive physical toll; understanding the impact of chronic stress on immune function is crucial for patient recovery and for the well-being of the healthcare workers fighting the disease on the front lines.
Despite the current lack of approved treatments, the scientific community is not standing still. Researchers are actively developing and testing immunotherapeutics. Monoclonal antibody therapies, such as m102.4, have shown significant promise in early clinical trials and animal models, offering hope that a targeted treatment may be available in the near future.
Effective Prevention and Control Strategies
In the absence of a vaccine, prevention remains the absolute most effective weapon against the Nipah virus. Preventive strategies must be implemented at multiple levels: individual hygiene, agricultural practices, and hospital infection control.
In regions where NiV is endemic, public health campaigns heavily emphasize food safety. The most critical directive is to avoid consuming raw date palm sap. If sap is to be consumed, it must be boiled first, as the heat effectively destroys the virus. Similarly, individuals should avoid eating fruits that may have been partially eaten by bats or contaminated by their droppings.
When preparing food, always wash and thoroughly peel all fruits before consumption. Any produce showing signs of animal bites should be immediately discarded. For more on building healthy eating habits and safe food preparation, checking out the complete guide to nutrition basics can provide excellent foundational knowledge.
Animal husbandry practices also require strict oversight. Pig farms must be designed to prevent fruit bats from accessing the enclosures or contaminating the pigs' food and water sources. If an outbreak is suspected in an animal population, immediate quarantine is necessary, and culling may be required to prevent human spillover.
Core Prevention Protocols:
- Food Safety: Avoid raw date palm sap. Wash, peel, and inspect all fruits for animal bites before eating.
- Hand Hygiene: Practice strict handwashing with soap and water, especially after visiting agricultural areas, farms, or markets.
- Avoid Animal Contact: Minimize unprotected exposure to sick pigs and areas where fruit bats are known to roost.
- Hospital Protocols: Healthcare facilities must implement rigorous infection prevention and control (IPC) protocols, including the use of gowns, masks, gloves, and goggles (PPE) when treating suspected cases.
Stay Informed and Protect Your Community
Knowledge is the first line of defense against zoonotic diseases. Share this guide to raise awareness about Nipah virus prevention, recognize the early symptoms, and keep your loved ones safe.
Share this content:
Discover more from J and J Health
Subscribe to get the latest posts sent to your email.